By 2030, the World Health Organization (WHO), the Global Fund and UNAIDS are hoping to end the human immunodeficiency virus (HIV) and AIDS epidemic.
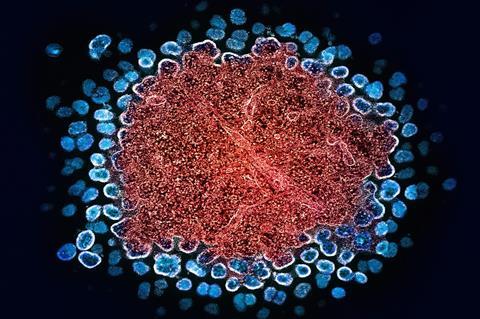
An international team of researchers led by Eric Arts, professor at the Schulich School of Medicine & Dentistry, and Jamie Mann, senior lecturer at the University of Bristol (U.K.), has brought us another step closer to meeting this goal, by finding an effective and affordable targeted treatment strategy for an HIV cure.
In a first, the study published in the journal Emerging Microbes and Infections demonstrated the team’s patented therapeutic candidate, an HIV-virus-like-particle (HLP), is 100 times more effective than other candidate HIV cure therapeutics for people living with chronic HIV on combined antiretroviral therapy (cART). If successful in clinical trials, HLP could be used by millions of people living around the world to free them of HIV. This study was done using blood samples from people living with chronic HIV.
Dead HIV particles
HLPs are dead HIV particles hosting a comprehensive set of HIV proteins that increase immune responses without infecting a person. When compared with other potential cure approaches, HLP is an affordable biotherapeutic and can be administered by intramuscular injection – similar to the seasonal flu vaccine.
“The development of this HIV cure was ten years in the making but with strong support from our collaborators in the U.S., Canada and Uganda, we have observed a striking ability of HLP to drive out the last remnants of HIV-1, which we hope will provide an affordable cure for all,” said Arts, who is a Canada Research Chair in HIV Pathogenesis and Viral Control. “To live HIV-free is a goal for the 39 million infected. It is also the priority of the UN and WHO to end the HIV pandemic by 2030.”
HIV is a retrovirus that attacks the body’s immune system and if left untreated, can lead to acquired immunodeficiency syndrome (AIDS). The virus weakens a person’s immune system by destroying CD4-T white blood cells, which are tasked with helping the immune system fight infections. Approximately 95 per cent of people living with HIV have chronic HIV – where the virus is slowly causing a slow destruction of the patients’ immune systems when they initiated lifelong cART.
Latent reservoir
While cART is effective at treating HIV, it has been unable to completely eliminate the virus from the body. This is because of the virus’ ability to create a “latent reservoir” – where it hides dormant inside of cells, safe from detection. Using blood samples from 32 participants living with chronic HIV from the U.S., Uganda and Canada, who were on stable cART for a median of approximately 13 years, researchers found that HLP was able to specifically target just the immune cells containing latent HIV reservoir and purge these cells of their HIV, a critical step towards an HIV-1 cure. An HIV cure is typically described as therapy and approach that eliminates all HIV without the need of continuous antiretroviral therapy.
“Over time, the virus grows more diverse within a single individual that is not on treatment which makes it more difficult to target,” said co-lead author Ryan Ho, master’s student in the department of microbiology and immunology. “This formulation we’ve crafted covers the theoretical diversity so it can reach the HIV-1 in all those people living with HIV.”
Minh Ha Ngo, lead author and postdoctoral scholar in the department of microbiology and immunology, says one concern expressed among people living with HIV for years is that continued use of cART could lead to the virus becoming unreachable and unable to be eliminated. The results of this study, by contrast, demonstrate that combining HLP with cART is still able to trigger the latent reservoir, even in chronic cases. If these dormant latent reservoirs can be awakened, then they can be eliminated from the body.
Global applicability
“Owing to its high mutation rate, HIV exhibits remarkable genetic diversity, resulting in different viral subtypes; some of which predominate in particular regions of the globe,” said Mann. “We were excited to see preliminary evidence that our HLP cure therapy reverses latency irrespective of the subtype of the individual’s infection. Whilst this needs to be explored further, it hints at the global applicability of our approach.”
In the future, researchers plan to test HLP on a larger representative HIV cohort with subtype C infections, which includes people living in South Africa, Ethiopia, Vietnam and India. This would help determine if the treatment strategy is effective for most people living with acute and chronic HIV.
These studies will be made possible with the advanced Pathogen Research Centre at Schulich Medicine & Dentistry. This study was conducted in collaboration with University of Bristol, University of Toronto, Case Western Reserve University, Rakai Health Sciences Program, Johns Hopkins University School of Medicine and the U.S. National Institutes of Health.
The study was funded by the American Foundation for AIDS Research, and by the Canadian Institutes of Health Research, U.S. National Institute of Allergy and Infectious Diseases; part of the National Institutes of Health, and the Canada Research Chairs Program.
Topics
- Case Western Reserve University
- Eric Arts
- HIV
- HIV-virus-like-particle
- Infection Prevention & Control
- Infectious Disease
- Jamie Mann
- Johns Hopkins University School of Medicine
- Minh Ha Ngo
- One Health
- Pharmaceutical Microbiology
- Rakai Health Sciences Program
- Research News
- Ryan Ho
- Schulich School of Medicine & Dentistry
- U.S. National Institutes of Health
- UK & Rest of Europe
- University of Bristol
- University of Toronto
- University of Western Ontario
- USA & Canada



No comments yet