Malaria, particularly in its severe forms, remains a global health and economic burden. It causes the deaths of more than 600,000 people every year – most of them African children under five. In a new study, published in the journal Nature, researchers from EMBL Barcelona, the University of Texas, the University of Copenhagen, and The Scripps Research Institute have discovered human antibodies that can recognise and target some of the proteins that cause severe malaria. This breakthrough could pave the way for future vaccines or anti-malaria treatments.

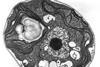
Severe malaria is caused by the parasite Plasmodium falciparum, which infects and modifies red blood cells. These modifications can make the red blood cells stick to the walls of tiny blood vessels in the brain. This results in impaired blood flow and blockage of small blood vessels, which causes brain swelling and can develop into cerebral malaria.
The blockage of blood flow is primarily driven by a family of about 60 virulent proteins, called PfEMP1, present on the surface of infected red blood cells. Some types of PfEMP1 proteins can attach to another human protein called EPCR on the surface of cells lining blood vessels. This interaction damages blood vessels and is closely linked to the development of life-threatening complications.
Increasing immunity
The researchers knew that when children in Africa grow older, they progressively develop immunity, and teenagers and adults rarely suffer from lethal disease complications. This protection was thought to be mediated by antibodies that target PfEMP1.
READ MORE: Maternal antibodies interfere with malaria vaccine responses
READ MORE: Malaria protein discovery offers path for novel antimalarial intervention strategies
PfEMP1 is a highly variable protein and has long been considered a technically difficult vaccine target. A long-standing question therefore has been whether the immune system can generate antibodies—proteins that recognise and neutralise specific pathogens—that can target the wide variety of PfEMP1 types in circulation.
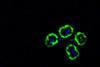
“We were hesitant whether we could identify a single antibody that could recognise them all, ” said Maria Bernabeu, co-senior author of the paper and Group Leader at EMBL Barcelona, “And it turned out that our improved immunological screening methods developed at University of Texas quickly identified two examples of human antibodies broadly effective against different versions of the PfEMP1 protein. They both targeted a part of the protein known as CIDRα1 which interacts with the EPCR receptor.”
Living blood vessels
The team then needed to test if those antibodies could also successfully block EPCR binding in living blood vessels. In most diseases, this could have been tested in animal models. However, for malaria, this is not possible because the virulent proteins of the parasites that infect mice are very different from their human counterparts.
The researchers came up with an innovative approach to overcome this challenge. They developed a way to grow a network of human blood vessels in the laboratory and to pass human blood infected with live parasites through the vessels, thereby reconstructing the disease in a dish. These experiments demonstrated that the antibodies were able to prevent the infected cells from accumulating, suggesting they might help stop the blockage that leads to severe malaria symptoms.
“We used our organ-on-a-chip technology to recreate brain microvessels in 3D, which we then infected with malaria parasites,” said Viola Introini, Marie-Skłodowska Curie postdoctoral fellow in Maria Bernabeu’s Group at EMBL Barcelona and co-first author of the work. “We introduced the two antibodies into the vasculature and were impressed at how well they prevented infected blood cells from sticking to the vessels. It was striking to see inhibition readily apparent by eye.”
Preventing parasite binding
Structural and immunology analysis by collaborators at the University of Copenhagen and The Scripps Research Institute revealed that these antibodies prevent parasite binding by a similar mechanism – recognising three highly conserved amino acids on CIDRα1. These broadly reactive antibodies likely represent a common mechanism of acquired immunity to severe malaria and offer novel insights for the design of a PfEMP1-based vaccine or treatment targeting severe malaria.
“This study opens the door to targeting new ways of protecting people from severe malaria, like a vaccine or other treatments,” said Bernabeu. “This is thanks to the international and interdisciplinary collaboration that is key to understanding diseases like malaria. Our collaborators are from across the globe, studying malaria from different angles. We have to continue working together to tackle big challenges like this one.”
She added: “At EMBL Barcelona, we believe that tissue engineering and growing organs-on-a-chip allow us to study diseases with much more complexity and detail, as well as provide useful platforms for screening vaccine candidates.”




No comments yet